Overview of Our Research
The central focus of our research is to understand how immune responses are regulated in tissues and how this knowledge can be exploited for therapeutic benefit. To this end, we currently have two areas of active investigation:
1. Understanding how regulatory T cells (Tregs) control immune responses in tissues
2. Understanding the ‘alternative’ functions of Tregs in tissues
Background
The mammalian immune system exists in a state of balance in which responses to an array of microbial antigens are permitted but reactions against self-antigens are suppressed. The establishment and maintenance of this balance is, in large part, the result of a finely tuned equilibrium between effector T cells (Teffs) and regulatory T cells (Tregs). Effector T cells eradicate microbial pathogens but can also cause damage when inappropriately directed against self, whereas Tregs control these responses.
It is becoming increasingly clear that tissues play a major role in regulating the immune responses that occur within them in an attempt to mitigate damage caused by inflammation and preserve organ function. The skin is a prototypical example. Many inflammatory skin diseases are characterized by defects in the ability to suppress pathologic immune responses occurring within the tissue. Alternatively, skin cancer results, at least in part, from an inability to mount productive anti-tumor immune responses. One of the main focuses of our research is to understand how this immune balance is established and maintained in tissues and how errors in this balance result in chronic inflammatory disease or cancer.
Our Approach
Because of its complex immunological properties, its accessibility, and potential for clinical translation, the skin is the model peripheral tissue that we currently study. Approximately 50% of our research employs a reductionist approach, utilizing transgenic animal models to ask fundamental questions of how the immune system functions in skin. The other half of our work focuses on doing functional immunology with human skin, human blood and humanized mice.
Research Related to Understanding How Tregs Control Immune Responses in Tissues
We have developed several animal models of skin inflammation that closely resemble human autoimmune and chronic inflammatory skin diseases. In one of these models, tissue antigen is expressed constitutively in the thymus and inducibly in skin, allowing us to precisely study Teff and Treg responses in a peripheral tissue upon induction of ‘self-antigen’ expression. Using this model, we discovered that self antigen-specific Tregs need to be activated by recognizing tissue antigens to become fully activated functional suppressor cells. During this process, some cells differentiate into long-lived memory Tregs, which provide continued protection against harmful autoimmune responses. We hypothesize that memory Tregs play an essential role in regulating tissue-specific inflammation and that defects in the establishment and/or maintenance of these cells result in chronic autoimmune and inflammatory disease.
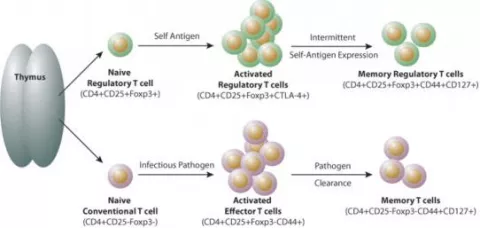
Lifecycle of regulatory and conventional CD4+ T cells. Naïve conventional CD4+ T cells and Tregs are generated in the thymus. Upon antigen-specific activation in secondary lymphoid organs, activated ‘effector’ T cells (both conventional and Tregs) are generated. Memory cells are generated from a subset of both conventional T cells and Tregs. These cells migrate to antigen-expressing tissues where they stably reside (tissue-resident memory cells) or recirculate between blood and non-lymphoid tissues (effector memory cells). It is currently unknown whether Tregs found in non-lymphoid tissues are comprised of tissue-resident memory cells or effector memory cells or both. It is also currently unknown if central memory Tregs are generated. (image from Ann. N.Y. Acad. Sci. 1283 (2013) 8–12 c 2013 New York Academy of Sciences.)
Current Projects Related to Understanding How Tregs Control Immune Responses in Tissues:
1. To define the cellular and molecular mechanisms responsible for memory Treg establishment, maintenance and function in skin as well as other peripheral tissues
2. To determine how the extracellular matrix (ECM) in skin influences Treg function, both in the steady state and during inflammation
3. Determine the cellular and molecular mechanisms that drive Treg accumulation in developing skin early in neonatal life
Research Related to Understanding the ‘Alternative’ Functions of Tregs in Tissues
Although previously thought to be a relatively homogenous population, it has become increasingly accepted that T regs are comprised of multiple subsets with unique functions. Perhaps the most distinct subsets are those that reside in peripheral tissues. Tregs found in tissues have unique functions. For example, in murine visceral adipose tissue, a subset of Tregs play a role in lipid metabolism and a unique population of Tregs is recruited into muscle after injury and facilitates tissue repair. The skin of both mice and humans contain a large percentage of the body’s Tregs. Currently, it is unknown whether Tregs in skin have tissue-specific functions, outside of their traditional role in suppressing inflammation. Preliminary data from our laboratory suggests that Tregs in skin play a role in: wound healing, hair follicle cycling, skin barrier homeostasis, and skin fibrosis.
Current Projects Related to Understanding the ‘Alternative’ Functions of Tregs in Tissues:
1. To define the cellular and molecular mechanisms by which Tregs in skin facilitate wound healing
2. To define the cellular and molecular mechanisms by which Tregs in skin facilitate hair follicle cycling with specific emphasis on epidermal stem cells
3. To define the cellular and molecular mechanisms by which Tregs in skin facilitate epidermal barrier repair with specific emphasis on epidermal stem cells
4. To define the cellular and molecular mechanisms by which Tregs in skin regulate fibrosis with specific emphasis on direct interactions with tissue fibroblasts
Translation to Humans
Although reductionist approaches utilizing mouse models are essential to elucidate fundamental mechanisms, a major limitation of these models is that some pathways shown to be critical in these systems do not translate to humans and/or human disease. Consequently, a major focus in the laboratory is the development and utilization of humanized mouse models. Humanized mice are genetically modified to be selectively immunodeficient, enabling them to accept human tissue and a human immune system. These animals allow for the study of human immune responses in mice and are proving to be a valuable tool for modeling human autoimmunity and chronic inflammation. The basic immunobiology of human tissue is readily studied in our models.
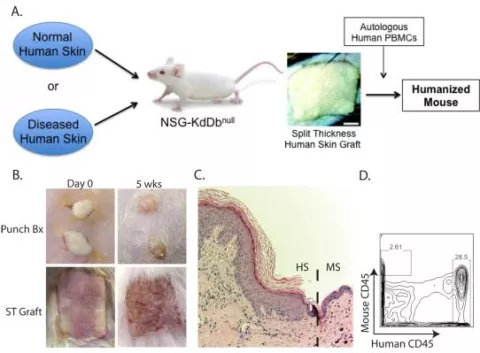
Humanized mouse model to study the human cutaneous immune system. (A) Overview of the humanized mouse system. (B) Clinical images of punch biopsies (Bx) or larger split-thickness (ST) human skin grafts on the day of grafting (Day 0) and at 5 weeks post-grafting (5 wks). (C) Histology of human skin grafts at 5 weeks post-grafting. Dashed line represents the intersection between human skin (HS) and mouse skin (MS). (D) Flow cytometry of a human skin punch biopsy graft at 5 weeks post-grafting showing the presence of a normal amount of human leukocytes and very few graft-infiltrating mouse leukocytes.
